After completing my 27-month physician assistant program, I accepted a job at a local urgent care company. When I received the first paycheck from my new six-figure salary, I remember thinking, “How could I ever want more money than this?” Unfortunately, I had never heard of The White Coat Investor and had no idea how to manage this money. My husband and I bought a new Ford Raptor that he had wanted for a few years. I convinced myself he “deserved it” after supporting me through school. This purchase, coupled with a prematurely inflated lifestyle of travel and luxury, changed my attitude toward the amount of money I was making. Suddenly, I was slightly envious of the multiple six-figure salaries the new doctors around me were making fresh out of residency.
I considered medical school while in college but ultimately decided against it after a brief experience shadowing a PA. I felt I could fulfill my desire for patient care as a PA while starting my life a little sooner. I wanted to get married, and I was not interested in putting off starting a family for 10 years through medical school and residency. Despite previously being confident in my decision, I began to wonder if I made the wrong choice based solely on the salary difference. This led me on a mission to earn more money.
According to the US Bureau of Labor Statistics, the average PA made $126,000 in 2022, while the average physician made $352,000 in 2023 (Medscape in 2024 said it was $363,000). These statistics are a little misleading since physician salaries vary greatly depending on specialty. For example, the average primary care physician makes a more attainable $277,000 a year. Using this number as our goal, I see at least three ways advanced practice providers (APPs), including PAs and NPs, can earn “doctor money.”
Practice Ownership
One clear path to making more money in medicine as an APP is to start and own your private practice. Our role in practice ownership lies mainly in primary care and urgent care. As an employed APP, you are paid a salary to see patients, generating revenue as your employer bills for your services. Your employer earns a profit if what they collect is more than your salary and the overhead it costs to run the practice. Cutting out the middleman means more food at your table.
The Need
Let’s just throw the cards on the table. To some physicians (and patients), the topic of APPs owning their own primary care practice is controversial. Some patients still don’t know the difference between a doctor and an APP. Some know the difference but don’t care, and there is likely a small minority of patients who prefer only to see a doctor. However, I believe most people want to see a provider who listens to their needs, who is knowledgeable in their medical decision-making, who projects confidence (not arrogance), and (most importantly) who is accessible.
Perhaps this controversy is becoming moot as the US is experiencing a severe shortage of primary care providers. A February 2024 article from CNN titled Where Are the Nation's Primary Care Providers? It's Not an Easy Answer illustrates the problem. In the graphic below, via KFF Health News, the bigger and darker dots show how big the healthcare professional shortage is in that area.
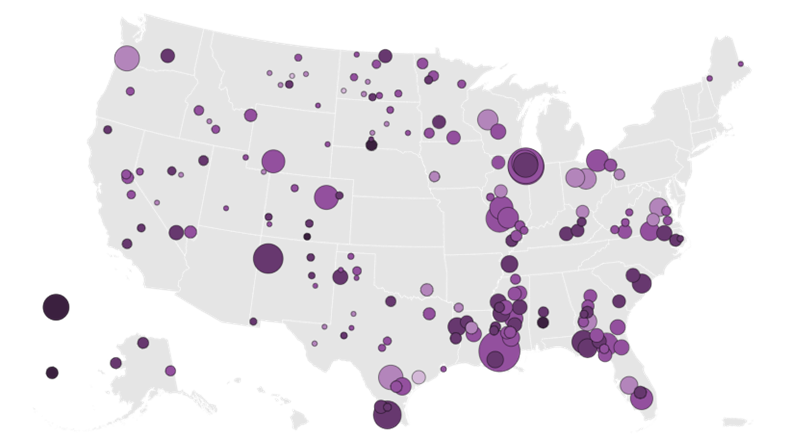
Geography, therefore, may play a pivotal role in whether APPs are accepted by the public as primary care providers and practice owners. In urban areas with an abundance of doctors, physician-led practices may have an advantage. However, in rural, underserved areas, APPs have an opportunity to step in and fill a healthcare need while building a profitable business.
What Practice Ownership Requires
Patience and Patients
Building a successful medical practice takes time and requires patience. You can't expect to leave your job making $150,000 and make that amount of money in your first few years of practice ownership. You might take a pay cut before seeing the fruits of your labor. It is also not a short game. When you open your practice, you sign up for at least 10 years of hustle. After all, when you own a family practice, you are the business.
You also need to see a lot of patients to make doctor money. This isn't the job where you will see 10-15 patients a day and make multiple six figures. Successful family practice owners need to see 30-40 patients daily to make the kind of money we’re discussing. Eventually, you might have the opportunity to hire another provider and be more flexible with your scheduling, but initially, it's all you. You have to expect to work hard.
Expanded Services
Over the years, primary care providers have been forced to see more patients in less time to make the same money, partially due to lower reimbursement rates from insurance companies. As a medical business owner, there are only two ways to make more money in primary care: see more patients or collect more per visit.
If you want to make doctor money but don't want to have to see 40 patients or more every day to do so, you can create other streams of income. It is common to see medical spas or hormone replacement therapy added into family practices to create recurring cash-pay patients.
At my website, we interviewed an NP whose primary business is a single-provider clinic in Midland, Texas. Over the past six years, Kevin has grown his family practice to 30-50 patients daily and has opened an adjacent medical spa as well.
Disadvantages of APP Practice Ownership
While owning your practice can be lucrative, it isn't easy. Owning and running a medical practice is hard work. And, like all investments, increased returns come with increased risk.
Hard Work
Successful medical practices require hard work. As you grow your practice, throw away your dream of an eight-hour schedule and expect long days and sleepless nights. Expect to work weekends in the clinic to attract more patients or to hold community events. Get used to seeing your shining face on billboards and TV ads, because, in a family practice, you are the business.
Financial Risk
Becoming a clinic owner will likely involve taking on debt to cover the office buildout, supplies, furniture, and medical equipment. In addition to upfront costs, you'll need to consider your ongoing expenses, including payroll, utilities, insurance (malpractice and benefits), and your office lease. Most landlords will want a five-year lease when you start, whether or not your practice is ultimately successful.
Medicolegal Risk
As providers, we all assume some medicolegal risk when seeing patients. As a business owner, you carry more risk, especially if you live in one of the 28 states with full practice authority for NPs or the five states that allow autonomous practice for PAs. Without a supervising physician, you are ultimately responsible for everything that occurs in your clinic.
Should this encourage you to still seek collaborative agreements with physicians, even if it is not required? Studies have shown that working in a private practice carries the greatest risk for malpractice claims when compared to other specialties. The AMA has shown physicians in solo practice tend to have the most malpractice claims against them, and the CNA and NSO have shown that NPs in an office practice are at the highest risk for license complaints against them, with 60% of claims being for violations of the scope of practice and standards of care.
One way to mitigate this liability risk is to still have a collaborative or supervising agreement with a physician. This will increase the financial requirement of owning your practice, as you can expect to pay $500-$2,000 monthly to your supervising physician. This number will vary widely depending on time requirements, expectations, and involvement from the physician. However, having a physician you can collaborate with on patient care is one step you can take to provide better patient care and to share liability responsibility.
Financial Upside: The Sky's the Limit
So, how much can you earn owning and running a medical practice? This will vary based on location, payer mix, patient volume, and services rendered, but ultimately, the sky is the limit. I know a local PA who owned his practice and regularly made nearly $300,000 a year before selling his practice to a physician-based group.
This amount is likely the ceiling with you as the only provider. After all, you can only see so many patients in a day. Eventually, you will need to hire other providers to work for you to make more.
[FOUNDER'S NOTE BY DR. JIM DAHLE: Like most physicians, I’m not a fan of the independent practice of APPs. I think a significant level of supervision is important to maintain a high level of patient care, particularly for new providers. However, it’s important to recognize reality on the ground. Twenty-seven states, mostly in the West and Northeast, have granted NPs the legal right to practice completely independently. Another 12, mostly in the Midwest, allow “reduced practice authority,” while the remainder requires total supervision. While PAs are required to have some level of supervision in every state, the degree of required supervision is highly variable. From an economic perspective, the cost of supervision can be a significant issue. You’re going to have a hard time finding a doctor willing to provide any real supervision for $2,000 a month, much less $500. However, the more supervision you desire or need, the less money you make. The incentive is to get as little supervision as possible—which can have both medicolegal and, more importantly, quality of care implications. Choose wisely.
That said, this is a COMPLETELY different issue from practice ownership. I’m a big fan of being an owner, whether it be your house, your investments, or your practice. While the vast majority of APPs are employees and not owners of practices, there’s no reason they can’t be. A physician can certainly offer ownership to an APP and vice versa.]
More information here:
Physician Assistant Financial Education
Life and Financial Lessons from a ‘Bad Ass’ Nurse
The Highest-Paying Healthcare Jobs
Hustle and Grind
The second way to make “doctor money” is to increase your workload. One of our greatest assets as APPs is career flexibility. You can use this to hustle your way to higher income. This will look different for everyone, depending on where you are in your career and life. It helps to start early when you have more energy, enthusiasm, and debt (and less money).
Logistics
If this is your strategy, pick a job that has a flexible schedule and shift work. For example, working in the ER or an urgent care facility may only require 10-14 monthly shifts to be considered full-time and receive benefits. This allows you half of the month to pick up extra shifts or get another part-time job.
Many remote or clinic jobs have flexible schedules if you want to avoid shift work. This flexibility allows you to find a second job to make additional money.
There are endless work arrangements available. For instance, I know a provider who works full-time in the ER and rounds on nursing home patients for a few hours every morning when he gets off. Another colleague works full-time as a fire captain as well as full-time in the ER. These arrangements bring two full-time salaries in exchange for grind and hustle.
The Downside of the Hustle
The biggest limiting factor is making sure you don’t burn out. I know very few people who can maintain this strategy for years. Most of us will reach a point where working 20+ days a month isn't feasible. I know a PA who made $250,000 a year working that schedule in urgent care, but they could only maintain it for a year or two. Hustle while you are young and hungry but expect you will one day reach your limit and tap out. The goal is to make some financial strides while you can still maintain the volume, pay off debt, learn to invest your money, and don’t overly inflate your lifestyle.
Financial Upside: Twice Your Current Salary
There are 168 hours in a week. Medical residents are legally capped at working 80 hours a week for a reason. Working more than this was shown to be counterproductive and dangerous. It's possible you could sustain 60 hours a week, earning 1.5x your current salary. Any more than this, and it's short-term only—with a theoretical maximum of 2x your current salary.
Entrepreneurship
The final way for an APP to earn doctor money is through entrepreneurship. This can include medical-related endeavors, such as opening a billing/coding company or a consulting business— or virtually any non-medical business you can think of. The possibilities and financial upside are endless, although my favorite method is real estate.
Starting and Running a Business
Finding a business you want to open is the first step. When I started down this path, I only knew that I did not want to do anything related to medicine. I already had a fulfilling medical career and wanted to try something new. Once I educated myself in personal finance and real estate investing, I opened a wholesaling business with the $20,000 we made from selling the Ford Raptor we had irresponsibly bought when I graduated. I learned about wholesaling by listening to the BiggerPockets podcast. I learned that you did not need an extensive amount of money for a startup, and you never had to acquire the property to make a profit. Growth and delegation are my two biggest struggles in this business currently, but I have learned what it means to be a business owner through the process.
One advantage you have as an APP is your above-average medical income, which you can use to start a business. Although maintaining a full-time job while running a business is certainly not easy, it is no different than options 1 or 2. Hard work is the recurring theme of making doctor money. When I started my real estate business, it was like I suddenly never clocked out. Every spare moment I wasn’t at work was spent working on my business.
Disadvantages of Entrepreneurship
Time
Other than the memes joking that entrepreneur is a synonym for unemployed Millennials, there are some real drawbacks to opening your own business. As an entrepreneur with a medical career, your workload will no longer be limited to your regular job. Your business continues running (and having problems) when you are trying to eat dinner with your family or going on vacation. Delegating tasks to others is the goal, but it usually takes time to get there. After 2 ½ years, I still have not gotten out of the day-to-day management of my business. I see the light at the end of the tunnel and I have witnessed this be successfully done in companies similar to mine, so I won’t lose hope that I can make this happen as well. But doubt occasionally creeps in. As an entrepreneur, fear of failure will be one of the biggest things you must overcome.
Risk
Like practice ownership, business ownership comes with a time commitment, financial risk, and even partnership risk. I ran our real estate business with my spouse for the first year and discovered how difficult it was for us to run a business together. We eventually decided for him to step away from the wholesaling business and focus on his own business as a real estate agent, which has been much better for our marriage. Friendships and relationships can be ruined unless clear boundaries are created and respected. You can make the wrong investment and lose a lot of money trying to make a business successful, or you can waste a lot of time and energy on a business that ultimately fails.
Financial Upside to Entrepreneurship: Unlimited
Entrepreneurship is high risk, but it can bring high rewards. The amount of money you can make is unlimited. Success is unlikely to occur overnight, but it is obtainable with education, hard work, and perseverance.
[FOUNDER'S NOTE BY DR. JIM DAHLE: A fourth way for APPs to make doctor money is to be more selective with your job and career selection. Just like with physicians, there is a very wide range of incomes within a given specialty, so it should be no surprise that the salary range of highly paid APPs overlaps with that of poorly paid physicians. Some fields, such as CRNAs, already enjoy physician-like incomes with salaries ranging from $190,000 (25th percentile) to $348,000 (75th percentile).]
More information here:
How I Made $30,000 Taking Doctor Surveys
Here’s the Best Way Ever to Get Passive Income – But Good Luck Getting It for Yourself
The Bottom Line
As an APP, I am thankful that I chose this career path. I don't envy doctors or their salaries anymore. I am grateful to have completed school and begun my career at 25 with under $100,000 in debt. But remember: whichever path you decide to take to make doctor money, none of it matters if you just spend it all. Plenty of physicians make multiple six figures but do not achieve financial independence because they spend all their money on their lifestyle.
It is important to understand that, as medical professionals, we have to take control of our financial lives through knowledge and disciplined financial management. Read blogs like The White Coat Investor and learn the basics of personal finance, investing, managing your taxes, insurance, and retirement planning. Pay off your debt quickly and efficiently, learn how to start investing your money to make money for you, and avoid prematurely inflating your lifestyle.
These are great steps to take in becoming FI—whether you’re a doctor yourself or a PA like me wanting to make doctor money.
If you're an APP, have you tried to increase your salary? What have you done? Has it worked?
